Alternative title: Pitching a VC on Disruption of Blood Testing
You may have seen some recent editorials about the necessary frequency of blood tests for healthy individuals, many of them prompted by a series of tweets from Mark Cuban:
Although there are certainly potential dangers in expecting any and all test results to be immediately informative and/or actionable, there are benefits in disrupting the status quo of how and when we collect information. A potential parallel is the “wearables” market, which has seeped from the “enthusiasts” (so-called quantified self-ers) to being used in trials of new drugs as well as disease research.
Blood Testing: Cost
One significant area of potential benefit to increased attention is cost. Generally when your physician prescribes a drug, you are asked what pharmacy to send the prescription. When told to get blood tests or imaging services, patients (in my experience) are sent to the affiliated providers. The burden is on the patient to ensure that the affiliate is covered by insurance. Even when they are, patients with high deductible plans (a growing number) are likely to become price sensitive IF there are straightforward ways to comparison shop and buy. Having gone through this exercise more than once myself, determining prices for medical services can be time consuming and frustrating, often at a time when money is the last thing you want to be worried about.
Although they have pushed their technological innovation as what allow it, pricing is apparently one of the main differentiators for biotech company Theranos (Forbes article; Theranos test/price list):
Its prices are often a half to a quarter of what independent labs charge, and a quarter to a 10th of what hospital labs bill, with still greater savings for expensive procedures. – Forbes
Theranos provides their tests through partnership with Walgreens, but there are companies that offer online blood tests directly to consumers, including WellnessFX, Direct Labs and most recently publicly traded Lab Corp (overview of the market from Bloomberg).
Blood Testing: Access
The players above are currently not available in all geographies as all require you to show up somewhere for the blood draw. In addition, in some areas, patients need a doctor to have blood work done. Theranos has also been vocal about the right of individuals to get blood tests without a doctor, for example supporting a recent change in Arizona law.
These companies aren’t the only ones looking to increase access to expensive blood tests. A much smaller company, Cue, is developing a system for at home testing of a small number of factors, such as testosterone or C reactive protein, using either saliva or blood droplets. The system is currently projected to ship to the first customers later this year. (Their FAQ has some additional information about their approach, including that the initial sales were done using an Investigational Device Exemption.)
Although Cue is focused on the consumer market, another medical trend, point of care testing in resource-limited environments, is driving progress in this space. Over the last few years, multiple research groups have described smartphone-based tools to run a lab test (specifically an Enzyme-linked immunosorbent assay or ELISA) that can be used for a wide range of diagnostic tests on blood. Some examples include research on infectious disease and cancer (here, here).
Quantified Self and Drug Dosing
I am not particularly interested in quantifying myself, but as a cancer drug developer and someone who has seen loved ones before, during and after chemotherapy, the possibility of (relatively) inexpensive and easily accessible blood tests is really exciting. Why? Because the way we determine the dose of cancer drugs a patient will receive has little to no relationship to “precision medicine”.
Dose is a straightforward way to refer to how much drug is given to a patient. However, the dose is not the only factor that contributes to how much drug a patient is actually exposed to. The same dose of drug may result in different exposure levels in the same person on different days and/or in different patients. There are a variety of common examples and two are provided.
For many calcium channel blockers (used to treat high blood pressure), the addition of grapefruit juice to a patient’s diet can increase the amount of the drug in the patient’s bloodstream. Grapefruit juice can have the opposite effect for other drugs, such as the cancer drug etoposide. In this case, a cancer patient might take a dose of drug shown to have benefit but the amount of drug in their body may be too low.
Some differences between patients can be traced to their genes. Some individuals have subtle changes in their genetic codes that alter the way their body breaks down drugs. The most common of these differences is in a family of proteins called the cytochrome P450 enzymes (CYP450). The dose of certain drugs, such as the cancer drug tamoxifen, may be modified based on genetic testing to determine how a patient metabolizes (breaks down) such drugs.
Coming back to cancer drugs specifically, getting the dose right is important because the therapeutic window (the difference between benefit and toxicity) tends to be much smaller than for other diseases. In the figure, you can see that as more patients have a benefit from the drug (traveling up the blue line), more patients are experiencing toxicity (traveling up the red line).
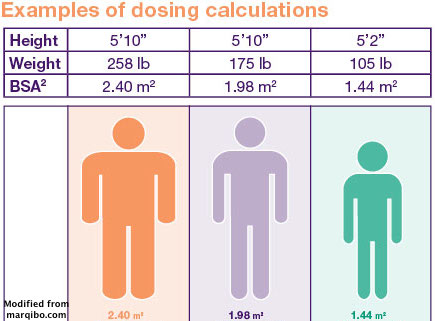
For oral cancer medications, the drugs are generally given in set doses (for example 100 mg of drug). Given what we talked about above, you probably aren’t surprised to hear that there is variability in the amount of drug patients “see”. (You can read more here if you have access.) A more opaque issue is that doses of many drugs (particularly chemotherapies given by intravenous infusion) are determined using something called body surface area (BSA), which is a formula based on a person’s height and weight. You can see that it is an attempt to “personalize” dosing. Unfortunately, the evidence suggests dosing by BSA is not the best way to achieve that goal. (You can read more here and if you have access here.)
Determining the amount of drug in the blood over time is called a pharmacokinetic assay and requires multiple blood draws as well as a way to detect the specific drug. While these tests are done during clinical trials, they are rarely a part of regular treatment regimens. There is a company called Saladax working to change that and bring cancer drug dosing into the era of personalized medicine with their MyCare tests. (I have no relationship with them but think it is very exciting.)
Although Saladax is working to bring these tests to health care providers, imagine an option down the road where you are able to test your cancer drug levels at home, accounting for all those variables of what you ate, the delay in taking the previous dose, etc. When we are working on the edges of benefit and toxicity, the ability to personalize doses could make a significant difference in quality of life for patients.
Knowing drug levels could also be helpful outside of oncology. Theranos can currently test for a handful of drugs, including tricyclic antidepressants. These drugs are an interesting example as going off of these antidepressants requires tapering, which is done using general timelines as opposed to actual blood levels.
Other Cool Things We Could Do With Blood
Expecting every test, every time to yield informative and actionable information is not the goal here. BUT driving down cost and increasing access to blood tests will allow scientists and clinicians to ask and answer questions we haven’t been able to before.
Monitor Nutrient Levels Remember Cue, the company that plans to let people test vitamin D levels at home? There are suggestions in the clinical literature that vitamin D deficiency lowers the efficacy of rituximab when given as part of a regimen for Diffuse Large B-Cell Lymphoma as well as worse survival in general for
patients with Follicular Lymphoma. Allowing patients to test various measures at home rather than only when at the hospital could lead to additional insights about improving diet during treatment or for overall health.
Optimize New Immunooncology Treatments One of the exciting new areas of cancer treatment involves getting the immune system to go after the cancer cells. Currently, blood work includes measuring a subset of immune cells called white blood cells, which includes the broad categories such as “lymphocytes” that counts all B cells and T cells. As our understanding of immunotherapy has developed, these populations of lymphocytes have been split into smaller groups and their impact on the response to therapy has been appreciated. Many immunooncology drugs are being explored in combination with drugs that can stimulate a good population of immune system cells. However, measuring these more defined cell populations, such as the regulatory T cells or the myeloid derived suppressor cells, is a much more complicated endeavor than a traditional blood panel. As a variety of companies are working on new instruments, pushing the cost of traditional blood testing down could help create room in the market for these newer, higher value tests.
Expecting every test, every time to yield informative and actionable information is not the goal here. BUT driving down cost and increasing access to blood tests will allow scientists and clinicians to ask and answer questions we haven’t been able to before. AND hopefully that will lead to better outcomes for patients in the short and long terms.









Reblogged this on The Digit@l Pillbox – Life Sciences Industry News & Trends and commented:
Very well written and insightful post about the use of blood in médicine. Worth a look!